Cancer is a disease so common that almost all of us have experience with it one way or another – whether it is as patients, friends, or family members. In 2020, 2.7 million people in the EU were diagnosed with cancer and another 1.3 million lost their lives to it.
The good news is that there is more hope than ever for cancer patients and their loved ones. Thanks to advances in digital technology and AI, we now have the tools to detect cancer earlier when it is more treatable, tailor treatments to the unique needs and characteristics of every patient to promote better outcomes, and support a better quality of life during and after treatment.
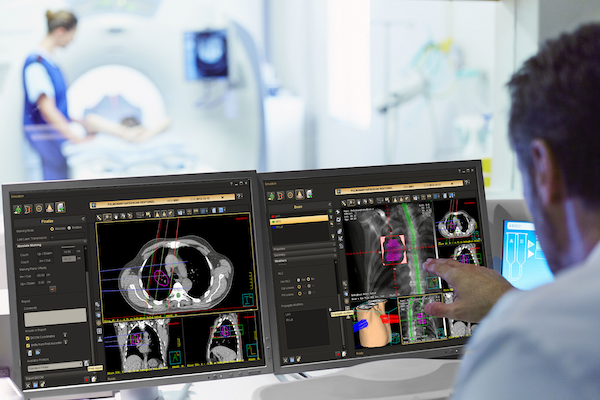
Unlocking insights from data
At the heart of the challenge – and the opportunity to accelerate innovation in cancer care – is data. Or more precisely: turning data into actionable insights.
Cancer care teams are collecting ever more information about patients, from medical imaging studies to pathology data, genomics, and data stored in electronic health records, as well as treatment outcomes. As the amount of data and the number of specialties involved continues to grow, so does the complexity in integrating and making sense of all this data. Adding to the challenge is that patients often see many different care providers throughout their care journey, with health data increasingly being collected at home and out of the hospital as well. Meanwhile, new treatments become available every day, presenting cancer care teams with a bewildering array of options.
At Philips, we are partnering with healthcare organisations worldwide to help them turn this information overload into meaningful insights at every moment in a patient’s care journey – from early screening and detection to diagnosis, treatment, monitoring, and follow-up, including care at home.
For example, together with clinical partners we have developed AI-enabled dashboards that can integrate different types of patient data to improve the efficiency and quality of multi-disciplinary tumor board meetings, while potentially saving up to 24% of the time spent per patient case. Following diagnosis and staging of the patient’s cancer, we can offer care teams patient-specific and evidence-based recommendations for therapies or clinical trials, building on our partnership with the world-leading Dana-Farber Cancer Institute in Boston.
Advanced data analytics and AI offer further possibilities to personalise cancer care. For example, as part of BigMedilytics – an EU-supported big data consortium led by Philips – we have investigated the potential of predictive models to help clinicians and patients make more personalised treatment decisions in prostate cancer care. Working in close collaboration with clinicians, hospital leaders, and patients, with the support of public funding, has been pivotal to the success of these pioneering efforts.
From innovation to implementation: overcoming fragmentation
Despite the promising results of such innovation programs, scaling them beyond initial pilot projects has proven to be challenging in Europe. That’s because the deployment of AI- and data-enabled solutions in clinical practice is hindered by the fragmented nature of European health systems.
Lack of interoperability and scale, complexities in data access, along with different health data processing rules across the EU all pose barriers. As a result, patients often receive fragmented care as they move from specialist to specialist – with potentially suboptimal outcomes – while cancer care professionals continue to struggle with inefficiencies.
What’s the remedy?
Data- and AI-enabled technology will only live up to its full potential in Europe if we overcome this fragmentation and establish interoperable data-sharing infrastructures at scale that make the necessary data available when and where they are needed. The current lack of such infrastructures puts a damper on AI innovation – which is doubly problematic as Europe is globally already lagging behind in AI capabilities.
The creation of common European data spaces could be a game-changer in many industries, including in healthcare where the European Health Data Space promises to enable more seamless data exchange. This will help pave the way towards a more integral, patient-centered approach to cancer care, as outlined in Europe’s Beating Cancer Plan – but only if the following three conditions are met.
First, the European Health Data Space needs to span the entire patient journey – making it easier for data to travel with the patient as they move between different departments, institutions, and care settings. To that end, the underlying governance framework should prioritise data standardisation and interoperability, building on internationally recognised standards to create a shared language for healthcare providers to connect and integrate data in meaningful ways. Consistency with GDPR is key, as is promoting further harmonisation in how it is applied across the EU.
Second, cloud-based platforms purpose-built for healthcare can provide the technological foundation to make data flow across healthcare systems, with the necessary privacy, security, and regulatory controls. To move beyond the current piecemeal approach in the adoption of cloud in healthcare, more European dialogue and transnational agreements are needed.
Third, to support adoption of digital innovations in cancer care at scale, reimbursement mechanisms should better reflect the value delivered to patients across their entire care journey.
Radical innovation of this kind requires a public sector rethink across many dimensions. In the fight against cancer, it could literally save lives and offer patients across Europe a brighter outlook for the future.

